“Eat What You Kill”
Lisa Warwick found her husband gasping for air at the foot of the basement stairs and knew the miracle was over. It was Aug. 2, 2020, more than 11 years since Scot Warwick had been diagnosed with Stage 4 lung cancer. Most patients are dead in months, but her husband, who had just turned 51, had somehow destroyed the odds.
“Are we going in?” she asked.
“Yes,” he said. “We are going in.”
His body had endured six years of chemotherapy and an additional five of experimental therapies. According to his medical record, he had responded “singularly impressively.” Two months earlier he had been running 5 miles a day, but since the latest round of chemo he had rapidly declined.
Lisa Warwick guided her husband up the stairs, dragged him to the car and raced to St. Peter’s Hospital in downtown Helena, Montana.
The emergency room doctor cited shortness of breath, fever and chills. He flagged that Warwick’s respiratory crisis could be the result of the chemotherapy. It had been restarted weeks before on the order of the oncologist who diagnosed him, the only doctor he’d consistently seen for more than a decade.
The next morning, a doctor named Randy Sasich arrived for his shift at St. Peter’s. An independent nonprofit with just under 100 beds, the hospital is the only acute-care facility for about 100 miles in any direction and has touched the lives of virtually every area resident going back generations. Helena, the state capital, remains a small vestige of the Old West, with just 34,000 residents, so luring doctors has always been a challenge. This was especially true in April 2020, at the onset of COVID-19, when Sasich signed a short-term contract.

Credit:
Brooke Herbert for ProPublica
A 47-year-old lung specialist, with degrees from Georgetown and Santa Clara University and experience at hospitals in major cities, Sasich was a rare get. The de facto director of the hospital’s intensive care unit, Sasich met with the morning shift’s coordinating doctor. Standing in the ICU, the two ran through patients, their needs, the usual, until Warwick.
We have a 51-year-old patient with metastatic lung cancer, diagnosed 11 years ago, Sasich remembered the doctor saying.
“There’s no way,” Sasich interrupted.
Well, he’s been treated for 11 years, the doctor explained.
“You don’t live 11 years after a Stage 4 lung cancer diagnosis,” Sasich said. “That doesn’t make any sense.”
Good journalism makes a difference:
Our nonprofit, independent newsroom has one job: to hold the powerful to account. Here’s how our investigations are spurring real world change:
We’re trying something new. Was it helpful?
Between patients, Sasich reviewed Warwick’s chart. Something must have been misread along a medical game of telephone, he reasoned, or he’d missed some great advancement in cancer treatment. He found the 2009 report that prompted the cancer diagnosis. A smoker at the time, Warwick had seen an ear, nose and throat doctor about a tiny lump on his neck. The ENT had sent a sample of cells from Warwick’s neck to the lab. A few days later he wrote in the file that they were “most likely consistent” with cancer.
That is not a cancer diagnosis, Sasich thought.
The records indicated that Warwick was referred to the hospital’s Cancer Treatment Center. Sasich’s curiosity graduated to shock: There was no biopsy. Yet Warwick was immediately placed on an aggressive chemotherapy regimen by the hospital’s sole oncologist, Dr. Thomas C. Weiner.
This is bad.
In his few months at St. Peter’s, Sasich had already questioned Weiner’s incomplete documentation and curious diagnoses and had taken his concerns to a veteran doctor for advice. To Sasich’s surprise, his colleague was fearful of challenging Weiner. According to Sasich, the doctor said: “I live here. My kids go to school here. I don’t want to move.”
Sasich scoured Warwick’s file, thinking someone must have ordered a lung tissue biopsy, which would capture more cells and target the suspected origin of the disease. Where was the lab report that confirmed cancer and ruled out everything else? From 2009 to 2019, he found none. Then, finally, there it was — in April 2020, just a few months earlier — a report on lung cells biopsied. Sasich read and reread the pathologist’s conclusion: no cancer.
“What the hell is going on here?” he whispered.
Despite the negative biopsy, Weiner had started Warwick on another round of chemotherapy, according to the medical records. Within two months, Warwick couldn’t walk upstairs, and now he was in the ICU while his wife and two children waited outside of the hospital because of COVID-19 protocols.
Sasich called the pathologist, who confirmed the finding. Sasich feared his own hypothesis. He worried what it would mean to Warwick and his family, but the “unbelievable conclusion” he had come to might save the patient’s life.
The next morning, Sasich entered the ICU where Warwick lay in the dark, oxygen pumping into his nose. Sasich pondered how to tell a man that everything he believed about himself for more than a decade was false.
Moments after Sasich left the room, Warwick called his wife. “He doesn’t know my history,” he told her. “He doesn’t know anything about me. He doesn’t know I’ve had this for 11 years. He doesn’t know anything. And this doctor’s telling me that I don’t have cancer? This guy’s an idiot.”
Sasich knew he had just challenged a powerful figure in Helena. He just had no idea how powerful.
While reporting on COVID-19’s toll in early 2022, I found myself in Helena, chatting over drinks with a handful of St. Peter’s medical staff. They wondered why I wasn’t asking about Tom Weiner. There was a deeper, haunting story, they told me, about the oncologist many inside the hospital suspected of hurting his patients. Despite those whispers, he was beloved by countless patients — “followers,” they called them. His nurses were wildly devoted to him — “a cult,” they said. The hospital administration feared him.
The rumors they shared, though vague, were disturbing and impossible to ignore. They portrayed a man whose ability to both inspire and intimidate had divided the town of Helena. It would take two years to unravel one doctor’s myth, a hospital’s complicity in creating it and the attempt to conceal a trail of suspicious deaths. One of them, I’d later learn, was of a 16-year-old girl.
Early in my reporting, I reached out to Weiner. Reluctant at first, he agreed to sit down with me. He was, he told me, the good guy in this story.

Credit:
Louise Johns, special to ProPublica
Weiner, 61, is guarded about his own life. He was raised Lutheran. His mother was a nurse, his father an FBI agent who urged him to be a lawyer. Weiner told me he was never much of “a research guy.” Rather, he wanted to bring a personal touch to medicine, to help people in their most vulnerable moments. He attended medical school at Hahnemann University, now Drexel, in Philadelphia. There, he met his wife, a devout Catholic, and he converted. An avid mountain climber and skier, Weiner felt that American westward pull and, after training in hospitals in Pennsylvania and Vermont, took the job at St. Peter’s in 1996.
He arrived as something of a savior. In an ad in the Great Falls Tribune, the hospital announced that it had hired a permanent oncologist to direct its new cancer treatment center, replacing a rotation of doctors who made often precarious commutes from Great Falls, Bozeman or Missoula. For most of the next 24 years, he was the only option for thousands of cancer patients. It’s not an overstatement to say anyone who had cancer or knew someone who had cancer in that time knew of Weiner.
He was instantly popular. Among his first patients was fashion designer Liz Claiborne, whose husband described Weiner as “a solid rock of a man, cheerfully youthful, robust, square-shouldered, handsome in a quiet way.” The Weiners became prominent members of the Cathedral of St. Helena and donated money to the Vatican.
In our talks, he was as Claiborne’s husband described, if weathered by a quarter century in the dry high country. He is fit, almost always wearing hiking shoes, a North Face T-shirt on warm days, a fleece in the cold. With sharp blue eyes, he smiles when he explains his medical judgment, projecting an absolute conviction in what he believes and has done.
Weiner’s stature rose with the cancer center’s. In late 2000, a news article reported that it was now treating about 250 patients a year. Three months later, the facility announced it would be adding six chemotherapy chairs, a library and a meditation center. An article in the Independent Record, the local paper, noted, “In the five years that Weiner has been with the cancer treatment center, he has seen an increase from 12 or 13 patients per day to 35 or 40 patients per day.”
Weiner told me, and records confirm, that he billed for as many as 70 patient contacts a day. That pace made him an obvious outlier in data tracked by federal insurance regulators, but no one inside or outside the hospital slowed him down. He spoke proudly of his workload. He was always on call, he told me, and many of his patients had his cellphone number. As business boomed, so did Weiner’s wealth.
Adding to a six-figure base salary, his pay was calculated by the number of relative value units, or RVUs, he billed on behalf of the hospital. The system compensates doctors using weighted values for certain types of visits or treatment. It works like this: A doctor might be paid $100 per RVU. A routine physical might be equal to 1 RVU, or $100; a more complicated and time-consuming procedure like radiation therapy might equal 8 RVUs, or $800. In other words, the more patient visits and treatments a doctor bills to insurance, the more that doctor and the hospital earn. Weiner described this system, which is common in American medicine, as “eat what you kill.”
In 2006, Weiner purchased a 3,400-square-foot home atop Mount Helena with a panoramic view of town. The next year, Weiner’s rising RVUs made him the hospital’s highest earner at $751,000, tax filings show. By 2010, Weiner was paid more than $1.3 million, more than three times the salary of hospital CEO John Solheim.
Around this time, according to court records, hospital administrators worried that Weiner’s pay could draw scrutiny from federal regulators for a violation of the Stark Law, which prohibits physicians who bill Medicare and Medicaid from referring patients in ways that enrich themselves. Those programs account for about 60% of St. Peter’s revenue. As questions about his pay intensified, Weiner responded by coordinating a staff rebellion, text messages show. A majority of St. Peter’s medical staff signed a letter of no confidence in Solheim, and Weiner was the lead signatory of a letter published in the Independent Record that charged the hospital with caring more about money than quality patient care. Not long after, Solheim resigned. He did not respond to my requests for comment. It’s unclear if the hospital at that time had its own concerns about the quality of Weiner’s care.
St. Peter’s had flourished since Weiner’s arrival, recording nearly 200,000 patient visits and bringing in more than $187 million in 2012. Weiner told me that most years his cancer care accounted for more than a quarter of the hospital’s revenue; St. Peter’s told me it was closer to 10%.
When negotiating his pay, emails show that Weiner leveraged his position as the region’s only oncologist, threatening to sue or quit, and he would prevail. With that power, he built a kingdom. In an unusual move, St. Peter’s allowed him to take over every facet of his patients’ care by naming himself their primary care physician. Because other options for cancer treatment were a long car ride or plane trip away, patients rarely sought a second opinion. Weiner protected his turf, resisting attempts to hire another oncologist or to transfer his patients to other doctors, court records show. As a result, few colleagues were looking over his shoulder. Inside the hospital, some referred to what he created as “his closed system.” As one doctor put it to me, if you were Weiner’s patient, “he grabbed on to you. He stayed with you for life. No one else would see you until you die.”
Concerns about Weiner’s billing and patient load persisted. Solheim’s successor, Nate Olson, also questioned his compensation. Weiner again helped organize a vote of no confidence, records show. Olson, who did not respond to requests for comment, stepped down in May 2016.
In 2019, St. Peter’s current CEO, Wade Johnson, hired an expert on the federal False Claims Act and fraudulent billing practices to study Weiner’s pay. The consultant described Weiner’s RVUs as “exceedingly high” and his compensation “a significant outlier.” Weiner logged nearly four times the visits and treatments of the median oncologist in the United States, despite working in a sparsely populated region. The consultant said the billings could be defended but warned they presented a potential legal and financial liability for both the hospital and Weiner.
From 2009 to 2020, the period Scot Warwick was under his care, the hospital paid Weiner more than $20.1 million. In all our conversations, he never shirked questions about his income. The bottom line, he told me, was that without him, St. Peter’s had no cancer center. “You want me to keep seeing everyone?” he said. “Then you’re going to pay me more, because I’m doing more work.”

Credit:
Louise Johns, special to ProPublica
Each morning Warwick lay in the ICU, Weiner visited, still dressed in his gym clothes. Over a decade Warwick had come to see his doctor as a friend. In their talks, Weiner dismissed Sasich’s hypothesis, though he agreed with the decision to stop administering the chemotherapy drug gemcitabine. As Sasich spent more time with Warwick, his confidence only grew. Throughout his treatment, Warwick had shown few symptoms of lung cancer and had continued to backpack, camp and kayak with his kids.
In Warwick’s records, a medically coded tit for tat ensued between the hometown celebrity and the outsider. Sasich ordered a new biopsy and tests to look for infection in Warwick’s lungs. “Dr. Sasich,” Weiner responded, “is still skeptical of the diagnosis.”
Lisa Warwick first heard from Sasich on Aug. 9, a week into her husband’s hospitalization. He wanted to explain the need for another lung biopsy. A habitual note taker, she scribbled words her mind could not accept: “This doesn’t present to me like cancer,” he told her.
“Well, how could that be?” she remembered thinking. “All our lives sucked for 11 years. I can’t imagine that we went through all that and it not be real.”
Sasich agonized about what to do. Doctors rarely challenge one another’s work. But after talking with the Warwicks, he filed an official complaint, accusing Weiner of an egregious mistake. He sent a letter to the hospital’s peer review committee, an internal group of doctors tasked with examining concerns about patient care. In it, he wrote that Warwick “would be the longest living case in the medical literature.”
One of the tests Sasich ordered indicated a possible fungal infection in Warwick’s lungs — not uncommon for patients whose immune systems have been wrecked. He was treated with steroids and an antibiotic cocktail. Warwick improved and, on Aug. 13, was sent home with an oxygen tank. Three days later, Lisa Warwick found him suffocating. He left home again for St. Peter’s, this time in an ambulance.
After a week of tests, Sasich called Lisa Warwick to tell her that her husband was experiencing a rare and excruciating reaction to the antibiotic Bactrim. Called Stevens-Johnson syndrome, it causes the skin to blister and peel. He was intubated and flown to a specialized burn unit at the University of Utah’s Huntsman hospital. The next day, Warwick’s left lung collapsed. A doctor told her to rush down to Salt Lake City.
For three weeks, Lisa Warwick lived at Huntsman, unable to leave and reenter because of COVID-19. Inside, doctors expressed to her confusion about Warwick’s diagnosis and sparse medical record.
When his right lung neared collapse, a doctor asked about his dying wishes — his code status. Do not resuscitate, Lisa Warwick said, a DNR. When they could do no more, the lead doctor pulled her aside. According to court records, he asked if she wanted an autopsy. As he asked, the doctor nodded his head up and down. She said yes.
Scot Warwick’s final communication with his wife was a faint squeeze of her hand. He died just after midnight on Wednesday, Sept. 16, 2020.

Credit:
Louise Johns, special to ProPublica
About a month later, his widow heard from the medical examiner. This is how she recalled the conversation during court testimony:
“Mrs. Warwick, I’ve never had to make this call before,” he said. She began to take notes. “I’m sorry.”
“OK?”
“We did not find any cancer cells at all. We can’t find anywhere in his records that he had cancer and found no malignancy at all.” All signs indicated he died from lung failure caused by the drug gemcitabine. Chemotherapy killed him.
As the conversation closed, she asked: “What am I supposed to do with this? What do I do?”
“Get a lawyer,” he said.

Credit:
Louise Johns, special to ProPublica
After Warwick’s death, Sasich bumped into Dr. Robert LaClair, the hospital’s kidney specialist and chair of the peer review committee. “How the fuck did this go on for so long?” Sasich asked. He considered LaClair an excellent specialist and consulted him frequently. From LaClair’s face, Sasich worried he had offended him.
A former Air Force doctor, LaClair has a certain respect for bureaucratic channels, which Sasich admits is not his domain. LaClair had worked with Weiner for 11 years and over that time had choked down his concerns. As he would later tell me: “I was caught up in the culture. We all were.”
LaClair revealed to Sasich that for months he had been quietly building a case against Weiner. According to court testimony, he advised Sasich to lay low as any attempt to remove Weiner had to be done “by the book.” Weiner had the money to sue the hospital and had threatened to do so many times. It could become a circus. Sasich was relieved that something was happening but was outraged that no one had acted before his patient suffered an agonizing death.
What LaClair didn’t tell Sasich was that the problem was worse than he knew. The review had begun a year earlier, after LaClair and a colleague questioned Weiner about his practice of providing minimal, often indiscernible, notes in his patient files. This poor documentation complicated follow-up care and, according to LaClair, intentionally made it difficult for others to question Weiner’s treatment. Court records show LaClair and his colleague also told Weiner to stop admitting scores of patients to the hospital for stays unrelated to cancer — stays that financially benefited him.
By early 2020, doctors and nurses had submitted enough confidential complaints for peer review to make LaClair act. He sent a half dozen patient files to medical experts at the University of Utah, but the conclusions had been delayed by COVID-19.
After Warwick died, St. Peter’s added his file for review. The doctor examining it quickly responded, thinking there must have been a clerical error: The packet didn’t include a biopsy to support the 2009 diagnosis. On Oct. 9, St. Peter’s received his analysis: “If he had cancer, this course of many years would be truly remarkable.” It went on, “The long-term treatment with toxic medications in the absence of a confirmed diagnosis of cancer is not reasonable.”
External reviews typically lack forceful language, perhaps by design. Medicine is nuanced, messy and rife with decision points and diverging paths, so doctors grading other doctors can sound deferential, even perfunctory. The eight Utah reviews were different.
Looking at a 2018 incident involving a 62-year-old man whom Weiner had diagnosed with throat cancer, a reviewer described several decisions as potential “malpractice” that led to an unnecessary two-month hospitalization. As with Warwick, there was no biopsy in the file.
Another review criticized what Weiner didn’t do. A 67-year-old woman with breast cancer had received chemotherapy and undergone a mastectomy and breast reconstruction. In a June 2019 check-up, Weiner noted “no evidence of any recurrence.” But records show that he didn’t conduct a breast examination. (Records show that this was a common failing in his breast cancer treatment.) Months later, the patient found a lump. A biopsy ordered at another hospital confirmed the cancer had been back for some time, which led to a second breast tissue removal, radiation and chemo.
“I’ve never seen so many cases of what we sent out that was not meeting standard of care. I’ve never seen that before, and I hope I never see it again,” LaClair would testify.
LaClair later told me, “When the Utah reports came back, it was like: ‘Holy fucking shit. This is going to suck.’”
On Oct. 15, 2020, St. Peter’s suspended Weiner and revoked his privileges. Banished from the kingdom he’d built over a quarter century, Weiner told me he felt only “blank.”
The hospital hired The Greeley Company, a health care consultancy, to scrutinize the records of dozens of additional patients, many of them dead. Weiner would be given an opportunity to defend himself and regain his job at an internal “fair hearing.”
Word of Weiner’s suspension devastated the nurses at his cancer center, the core group of women who called themselves “Tom’s wives” or his “girls.” They were the envy of nurses in other departments for the prestige of working for Weiner and for the perks. From 2005 to 2020, records show that he gave them at least $140,000 of his own money in bonuses and jewelry. Upon retirement, nurses could expect diamond solitaire earrings worth about $1,500. He invited them to his home for dinners and holiday parties. They messaged him regularly, wishing him well on his extended trips to Italy.
In the weeks following his suspension, they delivered food and sent supportive notes. They vowed to resist the administration. Weiner told them not to lose their jobs for him.
“I love you. I’m here. I’m so sorry. I’m praying,” nurse Emily Burton texted him.
“You can tell the girls I will be fighting,” Weiner responded. “But it will probably get bloody.”
To others, like nurse Meghan Giovenco, he expressed anger: “They are going for the jugular. Scum.”
When Weiner heard that Sasich questioned his work in front of his nurses, he texted a hospital administrator, “FYI put a muzzle on Sasich or else.”
News of Weiner’s suspension spread through social media and Helena’s shops and diners. Patients formed a Facebook group called “We stand with Dr. Tom Weiner.” He saved their lives, their spouses’ lives, they said. He remembered the names of their children and grandchildren. He was kind, brilliant. Dozens more joined, then hundreds and hundreds.
To those inside St. Peter’s, it resembled the campaigns that forced out the previous CEOs — only worse. Soon, the first of what would be more than a hundred small rallies was held outside the hospital. By ousting the region’s only oncologist, they contended, patients had been abandoned, consigned to long waits and a rotation of travel doctors. One sign proclaimed, “I WANT MY DR. WEINER, NOT THE SECOND STRING.” Their message spread to yard signs, bumper stickers and T-shirts. Supporters caravaned along Helena’s downtown, honking horns.




Credit:
Louise Johns, special to ProPublica
The hospital fired Weiner on Nov. 17, 2020. Johnson, the CEO, convened a meeting with the cancer staff, telling them Warwick’s death was “the tip of the iceberg.” He barred attendees from recording the meeting, court documents show, and the hospital’s chief nurse paced the room, instructing employees to put their phones away. All of Weiner’s patients should seek second opinions, Johnson said.
Johnson also told the staff, “Don’t be surprised if black suits show up.” Weiner’s nurses understood this to mean that federal law enforcement or the Department of Health and Human Services would be investigating. “He explained it to be suits — there were going to be suits coming into the office and asking for things,” according to the testimony of nurse Andrea Thies, who, despite Johnson’s orders, took notes during the meeting.
“You walked out of there feeling like, ‘Was I killing people?’” nurse Fallon Melby would later testify.
Three weeks later, St. Peter’s posted an astonishing disclosure on its website: “The issues we have identified include the following: harm that was caused to patients by receiving treatments, including chemotherapy, that were not clinically indicated or necessary; failure to meet state and federal laws associated with the prescribing of narcotics; failure to refer patients to other specialists for appropriate treatments; and failure to meet requirements associated with clinical documentation.”
It’s unclear if the hospital referred any of these issues to the state’s medical board or to state and local law enforcement.
Days later, Weiner sued St. Peter’s and its executives for wrongful termination and defamation.
Early in 2021, Sasich was pulled aside by Shelly Harkins, the hospital’s chief medical officer. According to Sasich’s court testimony, she apologized for getting him caught up in this mess.
She next confided a story that rendered him “physically ill.” Hospital administrators had for years harbored suspicion about one case, a 16-year-old girl who died suddenly under Weiner’s care. Sasich remembered Harkins providing few details but saying Weiner was frustrated that another physician was treating his patient. Once he regained control of her treatment, the girl didn’t live long. “She told me that he gave her two doses of propofol,” Sasich testified, “and she died.”
Sasich hoped it was just a rumor, an exaggeration. But when he asked LaClair about it, the person who knew more than anyone about Weiner’s practice didn’t refute the story but for one correction. It wasn’t propofol.
“No,” LaClair told Sasich. “He uses phenobarbital.”

Credit:
Louise Johns, special to ProPublica
In the days after Weiner’s termination, dozens of his patients came into the hospital asking for refills of oxycodone, morphine and other opioids. The doctors taking over Weiner’s caseload couldn’t find the prescriptions in St. Peter’s electronic system, according to court records, and Weiner’s patient files were little help. So they turned to a state database that logs all pharmacy opioid sales and discovered he had been writing prescriptions by hand, which bypassed internal hospital controls. To their shock, they found that many of his patients had been on dangerous levels of narcotics for years. The state agency that oversees that drug registry did not respond to a request for comment.
Often the patients seeking painkillers didn’t have cancer and had no documented need for them. Weiner had ordered them as their primary care physician. Many were struggling with addiction. St. Peter’s created a document for doctors to track the crisis in real time. Their notes included: “nonsensical” and “one of the worst indications for opioids. I’m still piecing this together …” and “Many years on methadone. Not clear why.”
Weiner told me the hospital manufactured these allegations to justify firing him, and he denied writing prescriptions by hand.
St. Peter’s assembled a committee of pain management experts to review more than 2,000 patient files. Dr. Kyle Moore, an addiction specialist, led the effort to detoxify patients. He found that Weiner rarely accounted for what doctors call morphine equivalents; essentially, he didn’t do the math to ensure that when patients received drugs at different intervals and strengths they didn’t add up to a lethal dose. Weiner denied this. In the narcotics tracking memo, Moore is quoted as saying Weiner’s prescribing was “a greater danger to the community than coronavirus.”
The full scope of Weiner’s prescription practices may never be known. The hospital alerted the federal Drug Enforcement Administration, which began an investigation, a spokesperson told me. But court records show no attempt by St. Peter’s to quantify the problem beyond its initial scramble to detoxify patients. St. Peter’s would not tell me if it searched for patients in the community who overdosed or died, nor would it say whether it reported what it found to the state medical board.
While the front-line doctors taking over patients were horrified, court records show hospital administrators and the peer review committee had been warned more than a dozen times, since at least 2018, that Weiner was overprescribing. I learned that staff who raised concerns expected to be yelled at or intimidated by Weiner. In 2019, two nurses and a pharmacist questioned a Weiner order to apply a fentanyl patch on a 93-year-old woman who was already on opioids and bobbing in and out of consciousness. A nurse texted Weiner to ask whether he was sure. Weiner responded, “Tell them put it on or I will rip their lips off.” Weiner told me this was “an inside joke.”
Federal regulators also failed to address alarming trends. An analysis of Medicare drug data shows that, from 2013 to 2020, Weiner’s volume of opioid prescriptions ranked ninth among all cancer doctors who bill the program. When it came to morphine, Weiner consistently ranked among the top five. In 2017, he prescribed more morphine than any other cancer doctor. The Centers for Medicare and Medicaid Services did not respond to questions.
Before St. Peter’s fired Weiner, the hospital sent five pain management cases to The Greeley Company. All were deemed inappropriate. One case was Sharon Dibble, a 75-year-old with many health problems, including kidney failure and chronic obstructive pulmonary disease.
On March 6, 2018, for reasons that were unclear to the reviewers, Weiner doubled her extended-release morphine from 30 to 60 milligrams twice a day, on top of an oxycodone regimen. Four days later, Dibble’s daughter found her limp, blue in the face, not breathing. Paramedics rushed Dibble to St. Peter’s, where she was kept on life support for more than two weeks. She died on March 27.
St. Peter’s said the cause was acute respiratory failure — her body starved of oxygen and shut down. The family believed her mounting ailments overtook her. But that’s not what happened, according to the Greeley review. Weiner’s “excessively large increase” in morphine, it concluded, “led to respiratory arrest and the patient’s demise.”
When I raised the Greeley review with Weiner, he called it “ridiculous.” He told me that he swapped short-acting pain medicines for long-acting but that Dibble’s morphine equivalent was unchanged — a claim contradicted by medical records and the hospital’s review of her death. The Centers for Disease Control and Prevention cautions against exceeding the equivalent of 90 milligrams of morphine daily and warns anything above 120 risks overdose. Records show Dibble’s daily regimen equaled 195 milligrams of morphine.
St. Peter’s never told Dibble’s family what it knew.
Five years after Dibble’s death, I shared the report with her son and two daughters. During his mother’s last days, Tom Dibble made the decision to stop life-sustaining measures. It was, he thought, her time to go. Now, he feels duped.
“Not only did this individual cause her death,” he said, referring to Weiner, “but it’s pretty apparent that this whole thing was being covered up. We were never given any knowledge that this took place, and we have to live with this decision.”

Credit:
Louise Johns, special to ProPublica

Credit:
Louise Johns, special to ProPublica
Six months after Weiner’s firing, the hospital conducted its fair hearing. As in a trial, witnesses testify, attorneys cross-examine, but a fair hearing isn’t public, and the judges are doctors — in this case, a panel of three from St. Peter’s. Held in a hospital conference room, the hearing took six days. On the first night, LaClair spelled out the allegations — Warwick’s death, the numerous misdiagnoses, the narcotics and more.
But that wasn’t the worst of it. The hospital also accused Weiner of overriding his patient’s dying wishes. If a patient wants CPR or a machine to keep them breathing, they elect to be a “full code.” Weiner, the hospital said, had a pattern of altering, without consent, a patient’s status from full code to a DNR/DNI, do not resuscitate and do not intubate. The hospital would not tell me if it pursued a complete accounting of what the fair hearing panel determined to be “a serious violation of the standard of care and medical ethics.”
At the hearing, nurse Addie Weidow described two events in which she witnessed a patient’s code status being changed without permission, including one where a patient nearly died before an intervening doctor sent her to the ICU. In another instance, Weidow testified, the chart of a patient who was full code suddenly read DNR/DNI. Following hospital protocol, nurses tried to attach a purple wristband, signifying her wish to die without intervention. When the patient refused the band, Weidow said Weiner told them to “hang the band on the doorknob and leave it be.” In other words, if her heart stops, don’t enter the room. Weiner’s nurses called it “a slow code,” Weidow testified.
When Weiner left town, Dr. Ashley Coggins managed his patient load, giving her a rare view into his closed system. She testified that “many nurses have come to me in the last several years, telling me that that was a standard practice of his — to just change people’s code statuses once they were doing poorly.” She added: “He was basically using his own judgment as the judgment for people to live or die. It’s horrifying.”
During the hearing, a hospital attorney asked Dr. Kerry Hale about the 16-year-old girl, the rumor that now haunted Sasich. Hale couldn’t recall the girl’s name but remembered she had a Wilms tumor, a kidney cancer that affects mostly children, and was being treated on the pediatric floor. Then, out of nowhere, Weiner transferred her to his oncology floor “and then orders for DNR, and then three doses of phenobarbital were given, and the patient died, I believe, that evening.” Phenobarbital is a barbiturate commonly used to treat seizures during alcohol withdrawal. In large doses, it is lethal.
When Weiner’s turn came, his lawyer asked for his account. His answer was clinical and unflinching. “Mom wanted her comfortable,” he said. “So, I transferred her to the oncology floor, and I gave her pain meds, phenobarbital, and she died later.” Neither the hospital nor Weiner’s attorneys pressed him for more details.
“Comfort” was a word Weiner used often in our conversations. If a patient dies as a result of his treatment, he told me, it’s not unethical if his intent was to provide comfort. In medicine, this is called the principle of double effect. First developed by the Catholic saint and theologian Thomas Aquinas, it’s a set of criteria by which a person can morally justify ending someone’s life. It stipulates that a harmful consequence of a medical treatment, such as death, is permissible if it’s a secondary effect of beneficial treatment, such as alleviating pain with drugs. “It’s for their comfort,” Weiner told me. “It’s not that I euthanize them.”
At the fair hearing, Weiner denied the hospital’s accusations. “Part of my problem is I have a good memory,” he said, “so I just remember things, and I probably should put more in the chart.” It wasn’t odd that he prescribed high-dose opioids, he said. He’s an oncologist, and his patients were suffering. Why was he giving painkillers to people who didn’t have cancer? For most of his tenure, he said, St. Peter’s didn’t employ a pain specialist.
As for his end-of-life care, Weiner said he always discussed the options with patients — “tens of thousands,” he estimated — before altering their status.
The panel unanimously rejected Weiner’s appeal.

Credit:
Louise Johns, special to ProPublica
Despite being fired, Weiner maintained his medical license. The law only required St. Peter’s to report his suspension — not what it knew — to the state medical board and the National Practitioner Data Bank. The medical board would not comment on whether it conducted an investigation into Weiner.
Rather than go into private practice or retire, Weiner decided to sue St. Peter’s, spending, by his own account, millions of dollars. He told me that he expected the hospital to settle for as much as $20 million because “they can’t let out what they did.”
By suing, Weiner exposed himself and St. Peter’s to pretrial discovery. Over the next three years, thousands of documents — text messages, patient files, financial statements, the fair hearing transcripts — were entered in court as evidence. Hours of depositions by doctors, nurses, administrators and Weiner were recorded.
Although at odds in every other way, Weiner and St. Peter’s had one common interest: concealing the evidence. Both parties successfully petitioned the court to seal nearly all the discovery. I was able to obtain it.
If the residents of Helena had seen those files, they would know how Weiner built a high-volume business that billed as much as possible to public and private insurance, all the while sending numerous patients through a carousel of unnecessary and life-threatening treatments. They would have learned that the hospital had financial incentives to look away.
Evidence of that high-volume business was hiding in plain sight, in data published by CMS. An analysis of Medicare Part B billing data shows that, from 2013 to 2020, Weiner billed for 40,000 15-minute visits, more than any other doctor — of any specialty — in the nation. The publicly available data offers just a glimpse of what St. Peter’s knew was a much bigger problem. “He’d see 15 patients in 30 minutes,” LaClair told me. This made Weiner rich and apparently missed the gaze of insurance regulators.
If Weiner was such an outlier, why did he never come to the attention of CMS? I reached out to John Hargraves, a data expert at the Health Care Cost Institute in Washington. CMS investigators, he told me, are looking for obvious fraud, such as doctors billing for more expensive work than they delivered. Instead, Weiner crammed in an extraordinarily high number of less expensive patient visits into each day.
When I asked St. Peter’s about what I had found, the hospital refuted none of it. It would not answer questions about Scot Warwick or Sharon Dibble or any other patients despite being given health privacy waivers signed by the families. CEO Johnson turned down requests for an interview. Andrea Groom, the hospital spokesperson, emailed a statement that broadly declined to comment, citing ongoing litigation. “We believe this situation is isolated to a single, former physician, and we remain confident in the exceptional care provided by St. Peter’s medical staff,” it said.
In a follow-up email, Groom wrote: “Dr. Weiner was a highly productive physician, but this was not necessarily alarming, given that he was the only medical oncologist treating cancer patients for a large service area during much of his time with St. Peter’s Health.” Patient satisfaction ratings were high, she said, and complaints were rare. Groom added that “there was no reason at the time for St. Peter’s to believe that Dr. Weiner was providing substandard care.”
In a court filing, the hospital told a judge it expects to be sued by more Weiner patients.
What the hospital’s response ignores is that St. Peter’s enabled and protected Weiner. As LaClair said in his deposition, Weiner’s colleagues didn’t stop him earlier “because we were afraid of him.” In court filings, St. Peter’s admitted that for years it knew of “serious concerns of physician colleagues and staff members with several patient deaths.” When I asked Weiner why the hospital would publicly accuse him of various types of malpractice but withhold its concerns about his end-of-life care, he said it’s because administrators knew what he was doing and even encouraged it.
Fifteen months before he was fired, Weiner and his nurses took over the hospital’s end-of-life care. I found an August 2019 text message exchange between the hospital’s chief nurse, Kari Koehler, and Weiner that made it official: “Are you still okay if all end of life patients go to onc[ology] even if they aren’t yours? I just feel like those nurses do it best!”
Weiner responded: “I agree!!”
By the summer of 2021, the pro-Weiner Facebook group had about 4,000 members. The hospital CEO was “evil,” “a true devil” and “puke.” The group campaigned successfully to have Weiner named “Helena’s Best Physician” in the Independent Record and raised the money to rent billboards that read “WE STAND WITH DR. WEINER.” When I asked Weiner why the town was cleaved in two over him, he smiled and offered a correction. “I wouldn’t call it 50/50,” he said. “More like 80/20.”
For Lisa Warwick and her two children, each Weiner sign was a reminder to keep silent. “I was worried about violence against us,” she told me. That summer, the family sued St. Peter’s for Warwick’s wrongful death. In her deposition, the widow said: “My children lost their father. I lost my husband. It wasn’t quick. It was long. And it was torturous. And it was terrible. And I would never, ever wish that on anyone — ever.”
In his depositions, and later to me, Weiner maintained that Scot Warwick had Stage 4 lung cancer for 11 years. The April 2020 biopsy that didn’t show cancer? The pathologist missed the spot where the cancer was, he said. In our conversations, Weiner said that the cancer had passed back-and-forth between Warwick’s two lungs.
“He was pretty advanced, though?” I asked. “Don’t you think it would be hard to miss?”
“Well, you would think,” he said. “I agree with you. I was kind of pissed off.”
What about the doctor in Utah who performed the autopsy? He also missed the cancer, Weiner said.
The Warwicks and St. Peter’s eventually settled the case for an undisclosed amount. Weiner was not held liable because he was a hospital employee. Neither the family nor their attorney have solved the mystery of why three private health insurers paid for 11 years of Stage 4 lung cancer treatment. None of the companies responded when I asked.
When I shared Weiner’s claim that 80% of Helena residents stood behind him, Sasich didn’t disagree. He drove past the protesters on his way to work. In the hospital, Weiner’s nurses barely looked at him. The billboard gave him chills. He couldn’t understand why people weren’t demanding answers.
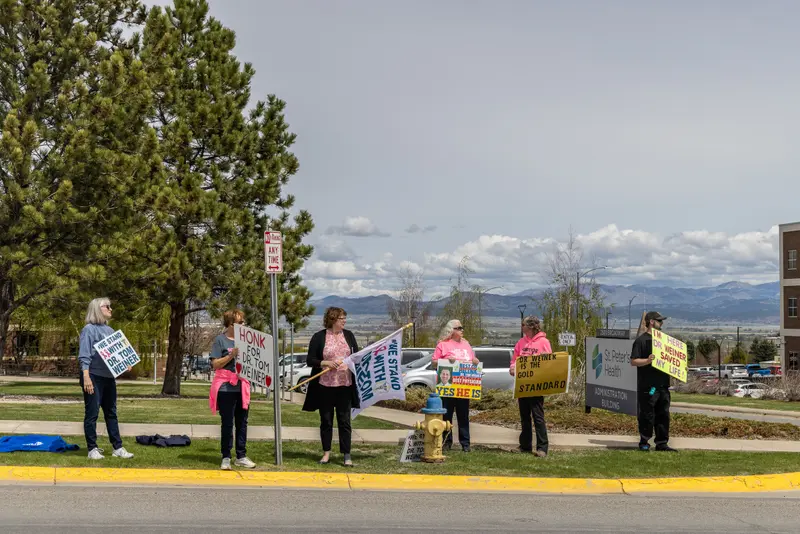
Credit:
Louise Johns, special to ProPublica
The mystery of the 16-year-old girl tore at him. He replayed the scenes in his head — Harkins, the chief medical officer, telling him that she may have been killed, LaClair confirming it. He asked a hospital attorney if they were investigating; “we’re aware of the case,” he was told. He took what he knew to Helena’s police chief. He had a brief meeting with a fraud investigator at the U.S. Department of Health and Human Services. No one seemed interested in pursuing it, Sasich told me.
Sasich’s inquiries came back to Weiner, who added him as a defendant in the lawsuit, accusing him of defamation. Sasich has denied the allegation.
Buried in the thousands of pages of medical records, correspondence and memos that build the hospital’s case against Weiner is a single sheet that summarizes the dying moments of seven people. In broken cursive, someone wrote in pen, “Phenobarbital cases.” Ranging in age from 53 to 77, they represent a small sample of those who died under Weiner’s care.
The memo tracks the final hours of a 62-year-old woman, admitted for stomach pain on Oct. 3, 2018. Four days later, at 6:01 p.m., she received 260 milligrams of phenobarbital for “terminal agitation.” Two hours passed. She received another 260 milligrams, then another at 10:58 p.m. — a total of 780 milligrams. She died just after midnight.
Unlike the narcotics and misdiagnosis cases, the hospital didn’t send these for outside review but rather enlisted its chief pharmacist, Starla Blank. During the fair hearing, Blank said the events were alarming because it wasn’t clear whether the patients were near death. “In most of the cases the patients were talking and visited with Dr. Weiner prior to their — prior to them getting the phenobarbital,” she said.
Still, St. Peter’s, which declined to comment on the phenobarbital cases, chose to ignore Blank’s assessment. In its final written account, the hospital concluded that the seven patients “were at end of life and that there were no remaining viable treatment options for them.”
One case is conspicuously missing from the phenobarbital memo.
There is no mention of the 16-year-old girl. In Harkins’ deposition, she recalled the case but not her name. LaClair’s testimony offered few details of an unnamed girl. Under oath, the hospital’s chief nursing officer referred to “a child” who had received so much phenobarbital as to arouse concern with nurses.
An online search of “Thomas Weiner” produces dozens of obituaries that express gratitude to the oncologist and his nurses for treating loved ones. One shows a photo of a thin girl with a big smile and blonde hair held back with barrettes. It speaks of hot air balloon rides in Arizona and beach trips in Oregon. She and her little brother built a play cabin in the woods and made pocket change selling lemonade. She loved camping and kayaking. At age 6, she was diagnosed with a Wilms tumor, but she didn’t let it rule her life. Her mother, who wrote the obituary, quotes her as saying, “Having cancer is no fun, but that doesn’t mean that you can’t have fun just because you have cancer.”
Her name was Nadine Long.
While I was reasonably sure this was the girl whose memory haunted the halls of St. Peter’s, I decided to knock on the door of the man who finally acted to stop Weiner but, by his own admission, had waited far too long.
To my surprise, Dr. Robert LaClair welcomed me into his home. Earlier that week in September 2023, a Montana judge had sided with St. Peter’s and thrown out Weiner’s lawsuit. The hospital had a right to enforce quality care under federal law, the judge ruled. In an addendum, the judge explained the hospital had not defamed the oncologist. Weiner vowed to file an appeal with the state Supreme Court. The judge did say, however, that Weiner’s defamation suit against Sasich could go forward. In LaClair’s study, we discussed Scot Warwick, the narcotics, the code status changes — cases he’d no longer have to recount in a trial. A weight seemed to be lifting from him, until I mentioned the name few knew. Taken aback at “Nadine,” his eyes welled. LaClair had read her file but had not sent it for outside review. He exhaled and after a long moment said: “Trust me, it’s so bad. You have no idea. She wasn’t terminal.”
By June 2024, Weiner and I had talked for many months. Sometimes, he’d offer an anecdote about an anonymous patient, unaware that I could identify their names and compare the stories with medical and court records. Invariably, he portrayed himself as a gifted and dedicated doctor. One was about a moribund young girl who needed him to intervene when a less capable doctor wasn’t keeping her comfortable. It was time to ask what happened to Nadine Long.
We sat at a long table in a hotel conference room in downtown Helena. Dressed in jeans and a short-sleeved polo shirt, he agreed to be recorded, attached a microphone to his lapel and talked first about a recent trip to Rome. Well into the interview, I presented him with a privacy waiver signed by Nadine’s family, and he told me his version of her final days.
It was March 2015. He was in New York, on Broadway, waiting with his wife for a matinee showing of “Les Misérables,” when Nadine’s mother called. She said her daughter was “in horrible pain. They won’t take care of her pain. Please come home.” After the show, he flew to Helena, arriving near midnight, and drove straight to St. Peter’s. Nadine was screaming and crying.
Weiner had treated Nadine since she was a child, when she was first diagnosed with cancer and when it recurred the following year. The cancer had now come a third time. Nadine had a pleural effusion — fluid built up between the lung and the chest cavity — that restricted her breathing. Her mother had talked with the oncologist filling in for Weiner, who was trying to transfer Nadine for further testing at St. Jude Children’s Hospital in Memphis, Tennessee. Weiner reviewed Nadine’s scans. “She was going down like a stone,” he told me. “She had hours to a day or two to live. There were no more cards to play.”
Hearing this, Nadine’s mother no longer wanted her transferred. “She just wanted her comfortable,” Weiner said. He gave Nadine a choice: a torrent of undignified treatments and pain with no promise of survival or “leave it up to God, and we’re just going to keep her comfortable.”
At that point, he moved Nadine to his oncology floor, to his nurses, “and she got some pain meds — I don’t remember how much phenobarbital — and she died later.”
His response mirrored what I had read in the fair hearing transcript. I had by then reviewed Nadine’s medical record, some of which I presented to him.
Weiner had examined Nadine less than a week earlier. In her file, he wrote, “she looks good … everything looks stable right now.” I asked how he could have missed what he claimed was an advanced and terminal disease.
“That’s how fast — the nature of that tumor when it comes back, it comes back with a vengeance,” Weiner said. “That fast.”
With her family’s consent, I had shared Nadine’s records with Dr. Sarah Friebert of Akron Children’s Hospital in Ohio. She specializes in pediatric oncology and founded and directs the hospital’s pediatric palliative care center. She wanted to be clear that she was not speaking for her employer.
I read aloud to Weiner some of her review.
“Here’s a girl who was skiing and then she’s dead a week later, and that’s — that’s concerning,” Friebert told me. “She ate 75% of her dinner on the night she died. Her vitals were not out of whack.” Nadine should have been sent to another hospital for testing, Friebert said, because nothing definitively showed she couldn’t have been treated. It’s not clear she was going to die, Friebert said.
Weiner determined she was dying based on a test of the fluid in her lungs, which was insufficient, she said. Neither Friebert nor I could find any evidence in Nadine’s file that Weiner ordered a biopsy that confirmed terminal cancer.
Friebert uses phenobarbital to calm children as they die of disease, but she told me Weiner “was escalating the phenobarbital in a way that is way out of proportion with what I would ever have done.” The intent, she said, could not have been comfort. “These doses were obscene,” she said. “He killed her with it.”
That a respected oncologist questioned his care didn’t seem to faze Weiner. She wasn’t there, he told me, and therefore can’t make such judgments. “I completely disagree,” he said. “This is a girl that’s got — her body is riddled with cancer, and she’s in horrible pain. Now did the phenobarbital hasten her death? Yeah, it did.”
In all our conversations, Weiner insisted his intent is always to provide comfort, never to hasten death, but here he equivocated.
“Could it have shortened her life?” Weiner asked. “Yes. Again, in most of these cases, could I not give phenobarbital, and would that patient live longer? The answer is yes.” Weiner paused. “But longer in, like, hours? I mean, is that worth being in misery for those hours?”
“My goal was not to kill Nadine,” he added. “My goal was to make her comfortable.”
I had shown him the “phenobarbital cases” memo, and we’d discussed the code status changes, Scot Warwick, the narcotics and now Nadine. Finally, I had to ask, “Are you killing your patients?”
“Well, uh, no. I’m not,” he responded.
“Why did you hesitate?” I asked.
“Well,” he said. “It depends on what you mean by killing them.”

Credit:
Louise Johns, special to ProPublica
Nadine’s parents live outside of Helena, at the end of a cattle road that curls around the peak where their daughter once played and her ashes now rest. Dan Beadle, her father, is an evidence technician for the county sheriff’s office. Her mother, Cheri Long, recently retired as an administrator at Carroll College in downtown Helena. They led me through the mudroom to the kitchen’s farmhouse table, where I asked them to recount the worst days of their lives.
While on a family vacation in New Hampshire in April 2005, Nadine was diagnosed with a Wilms tumor. She had her left kidney removed and received radiation. When the family returned to Montana, they met with Weiner, who directed her chemotherapy. During those treatments, Nadine bonded with his nurses, “the true loves of her life,” Long said. She appeared to be in remission. But a year later, the cancer reappeared in the spot where her kidney had been removed, Weiner told the family. Nadine received chemo and other treatments until about 2010, when Weiner said she was cancer free. She continued to see Weiner and his nurses for annual check-ups and more.
“Dr. Weiner always had a policy that once you’re his patient, he’s your primary physician,” Long said. “I don’t know if that’s normal.”
Nadine attended the same Catholic school as Weiner’s children. Her uniforms were hand-me-downs from his older daughter. The two families were friendly but not close. Nadine’s parents respected Weiner, although, as Long put it, he could be domineering.
Nadine also had bipolar disorder. When she was 14, a psychiatrist wrote that she struggled with information processing. He said her “insecurities, anxiety, and tendencies toward frustration when challenged dramatically interfered with her critical thinking skills.” But she was also “kind, compassionate, very empathic.”
In February 2015, Nadine’s parents noticed her hunching forward, struggling to breathe. She came to see Weiner on March 2. As with most of her visits, it lasted just a few minutes. “He listened to her lungs and said, ‘Everything’s good,’” her father recalled. “Then he tried to palpate a little bit, and she was extremely ticklish, so she started squirming around, and then at some point he goes, ‘I think we’re good to go.’”
Six days later, Nadine buckled and fell while skiing and was rushed to the St. Peter’s emergency room. Her parents were out of town when Nadine called to say: “Mommy, I’m in the hospital. My lung collapsed.” They raced to St. Peter’s, where they learned nurses had inserted a chest tube and drained her lungs of fluid, but no one would tell them more. Weiner was in New York City. For the next five days in the pediatric ward, Nadine vacillated between moments of calm and kicking and screaming, but her vitals were steady.
They felt they weren’t getting straight answers from Weiner’s backup oncologist. Long asked that Nadine be transferred to St. Jude. But as those arrangements were being made, Weiner appeared. “Finally,” Long remembered thinking, “We were like, ‘Someone who’s going to tell us the truth instead of tiptoeing around us.’”
She learned later that a St. Peter’s employee had phoned Weiner. His claim that he returned because Long called asking him to provide comfort to her daughter?
“That’s a flat-out lie,” she told me. “We did not ask for him to come home from his vacation.”
Weiner told her a large malignant mass was compressing Nadine’s lungs and would soon suffocate her. “How he described it was, ‘It’s doubling every day, and today it’s the size of a soccer ball,’” Long said.
Soon after, Weiner spoke with Nadine. “He spoke to our daughter, not to us,” Long said, “He told her, ‘You can choose the medical path or the God path.’” The conversation was “between the two of them. We were there, and he would check — he would look at us,” Long said. “Taking the God way was saying, ‘I fought my fight, and I’m ready to meet Jesus.’”
The teenager who struggled with processing information and critical thinking chose the God path. Her parents, terrified that she might needlessly suffer, didn’t object. On March 13, Nadine was changed from a full code to DNR/DNI, despite the day’s progress report that said, “She is alert and oriented, in no acute distress.” Weiner transferred her to the oncology floor.
Nadine had been heavily drugged since she’d arrived: Dilaudid, morphine, oxycodone, fentanyl. The next day, Nadine’s heart and respiratory rates elevated. She was panicking. “Saturday afternoon, she’s thrashing, she’s fighting, she can’t breathe,” Long said. Her father and a nurse couldn’t hold her down. They believed she was suffocating. The parents agreed to Weiner’s comfort measures.
Nadine’s medical file shows that he ordered a nurse to inject phenobarbital, which a computer tracked.
3:45 p.m. — 260 milligrams.
Nadine was still thrashing around. The nurse later said he was nervous about increasing the phenobarbital and called Weiner into the room. “He came in and stood there and oversaw,” Long said. “He just kept saying, ‘more, more.’”
5:26 p.m. — 390 milligrams.
It’s unclear when Nadine fell into sedation. After the initial doses, Weiner left the room.
7:47 p.m. — 390 milligrams.
Two of Weiner’s nurses who had doted on Nadine for years stayed late.
9:54 p.m. — 390 milligrams.
Relieved she was no longer in pain, her parents held on to her and each other.
1:45 a.m. — DISCHARGE.
Her heart stopped.
Nadine received 1,430 milligrams of a drug whose standard dosage for an adult is 260 milligrams. She weighed 100 pounds.
Nadine’s parents asked St. Peter’s to investigate the care she received. They wanted to know how Weiner could have missed a massive tumor a week before she died. Two months later, they met with the hospital’s director of risk management, who told them, Long said, “that he was reviewed and provided great care.”
For nine years, that answer had satisfied them. Believing Weiner had spared Nadine of pain in death, they put up a “We Stand With Doctor Weiner” sign in their yard. But now, having looked at Nadine’s medical file, they wanted to know if they had been manipulated, if she was actually terminal. Citing confidentiality laws, St. Peter’s has refused to provide the family the review, nor would it confirm to me that a review exists.

Credit:
Louise Johns, special to ProPublica
In August, Jesse Laslovich, the U.S. attorney for the District of Montana, and St. Peter’s announced a $10.8 million settlement for numerous violations of the False Claims Act: billing for unnecessary treatments, prescribing unneeded narcotics and more. The settlement, Laslovich said, “is not an indictment on the quality of care being provided by St. Peter’s Health as well as their doctors and their providers.”
The same day it announced the settlement, the U.S. attorney’s office sued Weiner. It accused him of getting rich by prescribing needless treatments, double billing, seeing patients more frequently than necessary and “upcoding” — billing for more expensive treatments than were delivered. The prosecutor pointed to Weiner’s enormous caseload as evidence that he had little regard for patient outcomes. Weiner’s attorney denied the allegations and has filed a motion to dismiss the case.
After the hospital reported Weiner’s narcotics practice to the DEA, the agency investigated, according to Steffan Tubbs with its Rocky Mountain field division. He told me investigators brought a potential criminal case to the U.S. attorney’s office but that prosecutors instead decided to pursue civil penalties against Weiner. A spokesperson for the U.S. attorney declined to comment.
In a press release, St. Peter’s commended itself for “acting with integrity” for alerting the DEA and laid blame on a rogue doctor. In settling, the hospital acknowledged that Weiner falsely billed multiple federal health care programs. But it did not acknowledge that his billing practices had been a constant problem and an obvious outlier for at least a decade. The prosecutor was silent on Weiner’s billing practices with private insurance.
The Montana State Supreme Court has yet to issue a ruling on Weiner’s appeal. His defamation suit against Sasich continues.
Weiner’s Montana medical license was renewed in 2023 and is set to expire in March. For now, he is free to practice medicine and prescribe drugs.
Neither the settlement nor the lawsuit against Weiner focus on the harm he exacted on countless patients. It’s unclear if any state or federal law enforcement agencies are looking into Weiner’s trail of suspicious deaths. Counting Scot Warwick, Sharon Dibble, Nadine Long and the seven documented phenobarbital cases, there are at least 10.
Mollie Simon and Haru Coryne contributed research and data analysis. Additional design and development by Allen Tan and Zisiga Mukulu.




